 Hallux valgus - the pathological crooked position of the big toe - is one of the most widespread "common diseases" among foot complaints. In the early stages, when there are only minor complaints, conservative therapy methods can be used for relief. These include, for example, shoe inserts, padding, hallux valgus splints, physiotherapy or painkillers. However, all of these measures can only alleviate the discomfort and in no way contribute to the elimination of the deformity. Surgical therapy is required for this. Depending on the stage of the hallux valgus deformity, various hallux valgus surgical methods are available. The chevron osteotomy presented here (Austin surgery) is only suitable as a surgical procedure for mild hallux valgus deformity and must be weighed individually. We provide information about other hallux valgus surgical procedures here.
Hallux valgus - the pathological crooked position of the big toe - is one of the most widespread "common diseases" among foot complaints. In the early stages, when there are only minor complaints, conservative therapy methods can be used for relief. These include, for example, shoe inserts, padding, hallux valgus splints, physiotherapy or painkillers. However, all of these measures can only alleviate the discomfort and in no way contribute to the elimination of the deformity. Surgical therapy is required for this. Depending on the stage of the hallux valgus deformity, various hallux valgus surgical methods are available. The chevron osteotomy presented here (Austin surgery) is only suitable as a surgical procedure for mild hallux valgus deformity and must be weighed individually. We provide information about other hallux valgus surgical procedures here.
Navigate to the individual points here:
For better understanding, we explain individual technical terms:
Osteotomy: Osteotomy is the surgical cutting of one or more bones with the aim of subsequent position correction.
Metatarsal: Located in the foot between the tarsus and the toes.
Forefoot: The metatarsal bones and toes are called the forefoot.
Stable under load: The patient can step fully in the bandage shoe directly after the operation.
Surgery according to Austin: First developed by Dale W. Austin and E.O. Leventen in 1962 in the USA.
Chevron osteotomy: This surgical method owes its name to the v-shaped incision technique. A "chevron" refers to a V-shaped American military insignia. The first use of a V-shaped osteotomy according to Kotzenberg on metatarsal was described by Schotte in 1929.
Sesamoid bones: The sesamoid bones are small roundish bones and lie below the 1st metatarsal head.
What are typical "slight" hallux valgus deformities?
A slight hallux valgus deformity is a crooked position of the big toe that is not yet very pronounced. The big toe is bent "inwards" so that the joint protrudes slightly at first. The angle between the first and second metatarsal is increased and small bony deposits form on the first metatarsal head. Hallux valgus is still in its early stages, but causes discomfort in the form of slight pain, swelling or shoe fit problems that trigger the desire for surgery. The appearance of the crooked big toe can also lead to patients preferring to have a hallux valgus operated on at this stage.
Visit private consultation now
When is this surgical procedure actually used?
The chevron osteotomy (surgery according to Austin) can be used for mild deformities. A further prerequisite is that the instability at the tarsal is only slight so that a symptomatic treatment approach is possible at all. The surgical procedure is not cause-oriented, as only the big toe is straightened. The chevron osteotomy (surgery according to Austin) is suitable for all groups of patients who are willing or able to accept fewer risks and inconveniences when undergoing surgery for hallux valgus. However, it is only recommended to a limited extent for a sustainable result, as the risk of recurrence (relapse) is increased.
Tonio Gottlieb, MD:
„In my experience, the chevron osteotomy (Austin surgery) is a quick solution to a mild hallux valgus deformity. However, I am generally more in favour of a cause-oriented solution that ensures a lasting improvement of the entire hallux valgus problem.”
For patients with hallux valgus, the foot surgeon Dr. med. Tonio Gottlieb is the designated expert on the subject of foot health and foot surgery. He examines you with the utmost care and always has the entire body statics in mind. Whether you need an initial diagnosis or a second opinion - make your personal consultation appointment now!
What exactly does surgery according to Austin or Chevron osteotomy mean?
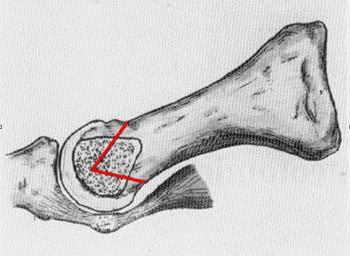
Chevron osteotomy takes its name from the v-shaped incision made during surgery. "Chevron" is therefore the description of the way the surgeon cuts through the bone - namely in a v-shape.
In Austin's surgery, the bone is also cut in a v-shape, but this surgical procedure includes other soft tissue interventions, depending on the findings. For example, the muscle is moved or the sesamoid bones are set.
Tonio Gottlieb, MD:
„The decision for a chevron osteotomy or surgery according to Austin must always be made very individually. Often I rather recommend a cause-oriented surgical method, where the patient has to put up with a little more discomfort after the surgery, but can expect a more sustainable result with a low risk of recurrence in the long term.”
What is the procedure for Chevron osteotomy (Austin surgery)?
 This surgical method involves a bony rearrangement of the first metatarsal. The head of the metatarsal is cut in a V-shape, moved outwards and usually fixed with a small titanium screw. This screw does not necessarily have to be removed again. The aim of the operation is to reset the metatarsophalangeal joint and the sesamoid bones. This is a symptomatic operation, as the actual causes of hallux valgus are not treated. These causes are usually instabilities of the entire statics, which have led to the metatarsal bones moving apart and can also lead to this happening again after a Chevron osteotomy (operation according to Austin). This hallux valgus surgery can be performed on an outpatient or inpatient basis. The decision always depends on the individual diagnosis and life situation of the patient. For older patients who live alone, an inpatient stay of a maximum of three days is recommended after the hallux operation.
This surgical method involves a bony rearrangement of the first metatarsal. The head of the metatarsal is cut in a V-shape, moved outwards and usually fixed with a small titanium screw. This screw does not necessarily have to be removed again. The aim of the operation is to reset the metatarsophalangeal joint and the sesamoid bones. This is a symptomatic operation, as the actual causes of hallux valgus are not treated. These causes are usually instabilities of the entire statics, which have led to the metatarsal bones moving apart and can also lead to this happening again after a Chevron osteotomy (operation according to Austin). This hallux valgus surgery can be performed on an outpatient or inpatient basis. The decision always depends on the individual diagnosis and life situation of the patient. For older patients who live alone, an inpatient stay of a maximum of three days is recommended after the hallux operation.
Tonio Gottlieb, MD:
„If there is instability in the metatarsophalangeal joint, the metatarsal slips over the sesamoid bones and causes pain. The principle of Chevron osteotomy (surgery according to Austin) is that the head is back over these sesamoid bones and the angle between the first and second metatarsal bone becomes smaller - so only the crooked big toe is straightened again.”
What is the healing process and aftercare like for this hallux valgus operation?
After hallux valgus surgery with Chevron osteotomy or surgery according to Austin, the patient must wear a bandage shoe for about six weeks and expect the healing time to be at least as long. The period of inability to work depends on the type of activity. In the case of a sedentary job, the patient can usually continue working immediately. For occupational activities with physical strain, a sick leave of at least six weeks must be expected. The bandage shoe is so stable that the patient can walk fully after the operation. No further walking aids are needed. Driving a car after a hallux operation is possible if the operated foot is not loaded (automatic transmission).
What exercises or physiotherapy help to speed up the healing process?
After the surgical wound has healed, the patient can already perform movement exercises independently. An additional visit to a physiotherapist is optimal for hallux valgus post-operative treatment. The physiotherapist can support the healing process with manual therapy, e.g. lymph drainage to reduce swelling in the joints or targeted movement therapy. After the bandage shoe has been removed, the foot is often still slightly swollen, so it may take some more time until the normal footwear fits again.
Can this type of hallux valgus surgery also be performed minimally invasively?
The hallux valgus Chevron osteotomy (surgery according to Austin) can also be performed in a minimally invasive way. In this case, the operation is performed through a small, approx. 1 cm long, skin incision.
Tonio Gottlieb, MD:
„Here, too, it must be decided on a case-by-case basis whether such a minimally invasive form of surgery is possible. It should be borne in mind that a larger skin incision often allows a better view of the surgical field.”
All important information on the surgical correction of mild hallux valgus deformities using Chevron osteotomy (Austin surgery) at a glance:
- Treatment type:
- Outpatient or inpatient (max. 3 days)
- Hallux valgus surgery duration:
- 30 - 60 minutes
- Hallux valgus surgery
aftercare: - 6 weeks Bandage shoe elevated (i.e. the crookedness of the big toe may return).
- Stability:
- Full weight-bearing, the foot is immediately stable under weight-bearing (i.e. in the dressing shoe, the patient can step out fully immediately after the operation).
Why should a mild or moderate hallux valgus deformity be performed by a designated foot surgeon and experienced food specialist?
 For a lasting hallux valgus treatment, it is always advisable to consult a specialist in the field of foot surgery.
For a lasting hallux valgus treatment, it is always advisable to consult a specialist in the field of foot surgery.
-
- Only a timely and reliable diagnosis can prevent further damage. Once a hallux valgus has developed, this pathological crooked position of the big toe cannot be reversed on its own. On the contrary, the deformity will tend to increase over time.
- An untreated hallux valgus not only causes discomfort and pain, but can also be responsible for further diseases. The late consequence is often arthrosis of the metatarsophalangeal joint of the big toe, which can lead to the inability to walk.
Therefore, hallux valgus should always be diagnosed and treated by a foot specialist.
For all hallux valgus symptoms, the experienced foot surgeon Tonio Gottlieb, MD, is your ideal contact and can recommend various surgical and conservative therapies for the treatment of a bunion. With an individual treatment plan, the chances of success for hallux valgus are very good. The chevron osteotomy (surgery according to Austin) presented here can also be performed by him - if indicated - in an uncomplicated and successful manner.
Tonio Gottlieb, MD:
„Try hanging the shutters on the leaning tower of Pisa straight. That is only possible if the entire statics of the tower are restored. That is why I always pay attention to the entire body statics with every hallux valgus diagnosis. This is the only way to achieve a truly sustainable treatment result for the patient.”
The foot surgeon Tonio Gottlieb, MD, is your experienced expert in the field of foot surgery and foot orthopaedics with a private practice in Berlin. He examines you with the utmost care and always has the entire body statics in mind. Based on a cause-oriented diagnosis, he will give you an individual, stringent recommendation for action. Whether you need an initial diagnosis or a second opinion - make an appointment for a personal consultation!


